Stopping depressive relapse is a significant purpose within the administration of bipolar dysfunction. It has been proven that melancholy makes up round 72% of general time spent sick in individuals with bipolar (Forte et al., 2015), and that bipolar melancholy particularly is related to important bodily and psychological morbidity, in addition to elevated mortality (Baldessarini et al., 2020).
Lithium is the first-line really useful remedy for stopping bipolar melancholy (NICE, 2014). Nonetheless, as a earlier Elf weblog has highlighted, prescription of lithium is declining, each within the UK and different nations (Edward, 2019). Antipsychotics, different temper stabilisers and – though not really useful by NICE – antidepressants are additionally usually prescribed long-term for individuals with bipolar dysfunction. As lately blogged right here and right here, using antidepressants within the long-term administration of bipolar dysfunction is controversial, with the chance of temper destabilisation related to antidepressant monotherapy, and it is suggested that they need to be prescribed for sufferers with bipolar dysfunction solely in particular medical situations (McIntyre et al., 2020; Pacchiarotti et al., 2013).
In a paper lately printed in The Lancet Psychiatry, Ermis et al (2025) aimed to check whether or not the prescription of medicines utilized in bipolar melancholy have an effect on the possibilities of sufferers with bipolar dysfunction being admitted to hospital because of a depressive temper episode.

Stopping depressive relapse is a significant purpose within the administration of bipolar dysfunction.
Strategies
Ermis et al used a cohort examine design to determine whether or not prescription of temper stabilisers, antidepressants and antipsychotics (prescribed and disbursed) have been related to admission to hospital attributable to depressive sickness (main consequence), and admission to hospital attributable to mania or a somatic situation (secondary outcomes). Topics and consequence knowledge have been recognized from ICD-10 codes (WHO, 2019) in Swedish nationwide registers from 2006-2021, while knowledge on topics’ drugs have been gathered from the Prescribed Medication Register.
A within-subjects Cox regression evaluation (adjusted for time-variant covariates similar to time since cohort entry and use of different psychopharmacological drugs) was used to check durations of time during which the topic was prescribed a particular remedy towards instances during which no antidepressant, antipsychotic, or temper stabiliser have been prescribed. Quite a lot of sensitivity analyses have been additionally carried out, to make sure the robustness of the findings.
Outcomes
105,495 individuals with bipolar dysfunction have been included. The imply age of the pattern was 44.2 years (normal deviation, SD 18.8), and 62.2% of the pattern recognized as ladies. Comorbidities have been current in a big minority (anxiousness problems 40.5%, substance use dysfunction 18.8%, character problems 10.4% and former suicide try 10.6%).
Comply with-up was commenced from the date of bipolar prognosis and the imply follow-up time was 9.1 years (SD 5.1). At follow-up, antidepressant monotherapy was the most typical publicity (utilized by 59,963 topics, 56.8% of the cohort, sooner or later in the course of the follow-up interval), adopted by temper stabiliser monotherapy (47,931, 45.4%) and antidepressant-mood stabiliser mixture (46,318, 43.9%).
General, 16,190 topics (15.3%) have been hospitalised with a depressive episode a minimum of as soon as in the course of the follow-up interval; 8,066 topics (7.7%) have been hospitalised attributable to mania.
Decreased probability of depression-related hospitalisation
- Temper stabiliser monotherapy was the one remedy group discovered to be related to a decreased probability of depression-related hospitalisation in contrast with the prescription of no drugs in any respect (adjusted hazards ration, aHR 0.89, 95% confidence interval, CI 0.81 to 0.98).
- Temper stabilisers mixed with antipsychotics have been related to a touch decreased probability of depression-related hospitalisation, however this was not statistically important (aHR 0.92, 95% CI 0.85 to 1.00).
- In particular person remedy evaluation, solely lithium was related to a decreased probability of admission attributable to melancholy on this cohort of individuals with bipolar dysfunction (aHR 0.75, 95% CI 0.67 to 0.85).
Elevated probability of depression-related hospitalisation
- Other than temper stabiliser monotherapy and temper stabilisers mixed with antipsychotics, all different remedy teams, both alone or together, have been discovered to be related to an elevated probability of depression-related hospitalisation.
- Notably, a number of drugs have been related to an elevated probability depression-related hospitalisation, specifically quetiapine, duloxetine, citalopram, olanzapine, mirtazapine, vortioxetine and aripiprazole.
Decreased probability of hospitalisation attributable to a somatic situation
- When it comes to secondary outcomes, lithium was the one remedy related to a decreased probability of hospitalisation attributable to a somatic situation (aHR 0.86, 95% CI 0.80 to 0.93), with no statistically important associations being discovered between the opposite drugs and somatic hospitalisation.
Elevated probability of mania-related hospitalisation
- Antidepressants-only have been the one group that have been related to elevated possibilities of hospitalisation attributable to mania (aHR 1.22, 95% CI 1.03 to 1.44); all different drugs teams, alone or together, have been related to decreased possibilities of mania-related hospitalisation.
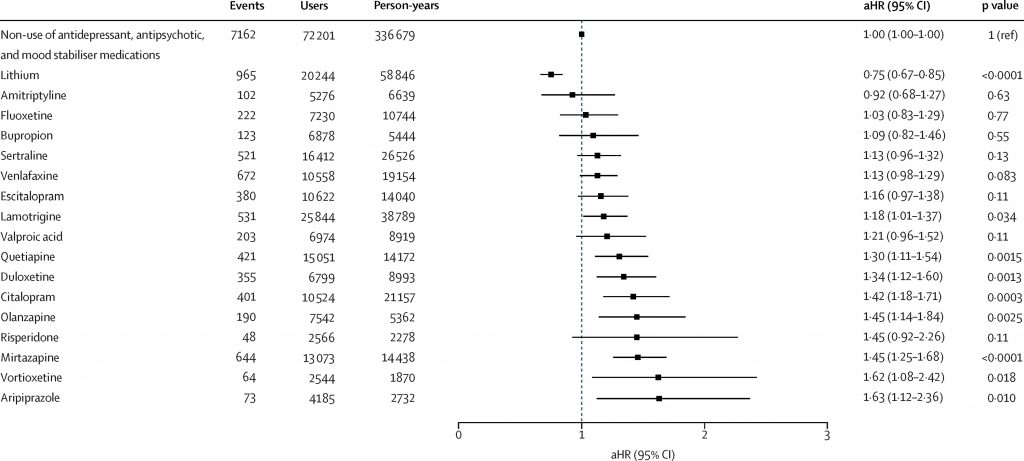
In particular person remedy evaluation, solely lithium confirmed a decreased probability of depression-related hospitalisation; all different drugs have been both equivocal or related to elevated probability of depression-related hospitalisation. [View full sized graphic]
Conclusions
The outcomes of this examine spotlight that lithium is the one monotherapy that decreases the possibilities of depression-related hospitalisation in individuals with bipolar dysfunction. Extra advantages have been additionally seen within the possibilities of mania-related and somatic hospitalisations, emphasising lithium’s multimodal advantages.
In distinction, sure antidepressants and antipsychotics have been related to elevated probability of depression-related hospitalisation.
“Present findings supported the notion that lithium ought to stay the mainstay of remedy in bipolar dysfunction” – Ermis et al, 2025
Strengths and limitations
A cohort examine design was the fitting methodology to reply this query. Cohort research, of their observational nature, enable researchers to determine the impact of exposures in pure environments, making the outcomes extra generalisable to real-life conditions. It additionally allowed the authors to check a number of drugs on the similar time, which might not have been potential to the identical extent in, for instance, an RCT design.
The examine inhabitants was taken from Swedish nationwide registers and ICD-10 codes have been used to establish these with bipolar dysfunction and the outcomes of curiosity. The outcomes are due to this fact reliant on appropriate utility of the ICD-10 standards at time of prognosis and proper coding of prognosis into the well being registers. Inside these limitations, the authors have been capable of pattern a lot of the inhabitants with a bipolar prognosis and supply follow-up over a number of years.
When it comes to the pattern demographics, charges of psychiatric comorbidity and suicide try historical past have been excessive, however this echoes the broader bipolar inhabitants (as highlighted by a earlier Elf weblog) and improves the generalisability of the outcomes from this pattern to real-world medical settings. It’s notable, nonetheless, that there have been twice as many ladies than males, which isn’t reflective of bipolar dysfunction’s 1:1 male-to-female distribution and that knowledge on ethnicity weren’t accessible, each of which restrict the generalisability of the examine outcomes to specific teams.
The authors famous that by specializing in hospitalisation, the outcomes of this examine are solely related for probably the most extreme circumstances of bipolar melancholy and don’t contemplate the advantages or harms that these drugs could also be exerting in sufferers who’re managed totally as outpatients. Hospitalisation is an goal, binary measure that has important real-world implications for sufferers, and so it may be argued that it’s nonetheless a superb measure of the efficacy of those drugs.
A remaining vital consideration is that use of registry knowledge doesn’t at all times correspond precisely to behavior. In different phrases, simply because a prescription was written, doesn’t imply the remedy was taken. Usually talking, nonetheless, it’s possible that almost all of these prescribed a medicine do take it, and the big numbers included on this pattern are more likely to minimise the impact that remedy non-compliance in small minority might have on general outcomes.

Regardless of limitations, the big pattern measurement and lengthy follow-up make the outcomes pretty generalisable to the bipolar inhabitants and vital medical situations.
Implications for observe
This paper reaffirms the standing of lithium as “the best long-term remedy for bipolar dysfunction” (NICE, 2014). As such, it’s regarding that the charges of lithium prescription look like declining (Lyall et al., 2019). The explanations for this are unclear, however, as a earlier Elf weblog highlights, it could possibly be attributable to anxiousness amongst sufferers and clinicians concerning the elevated monitoring that’s required for lithium or attributable to its particular antagonistic impact profile. It could even be associated to the low value of lithium, which can be driving the pharmaceutical trade to promote using different, dearer choices, doubtlessly swaying affected person choice. Regardless of the motive, a transfer away from prescribing lithium poses the chance of many sufferers lacking out on its potential advantages.
After lithium, the second- and third-line NICE-recommended preventative drugs for bipolar dysfunction are antipsychotic monotherapy and augmentation with valproate. This paper confirmed that these drugs have been related to reductions in mania-related hospitalisation, however no such profit was seen with depression-related hospitalisation. Some antipsychotics have been in actual fact related to elevated probability hospitalisation attributable to a depressive episode. This will make clinicians assume twice about prescribing antipsychotics or valproate long-term in bipolar dysfunction if the first intention of remedy is to forestall additional depressive fairly than manic relapses. In lots of sufferers this would be the intention, significantly as melancholy makes up nearly all of sickness time in these with bipolar dysfunction (Forte et al., 2015).
So, on the very least, Ermis et al have demonstrated the necessity for additional analysis on this space in order that we will make clear whether or not present medical tips for prevention of bipolar relapse are match for objective for all sorts of temper episodes, particularly in these for whom lithium shouldn’t be an possibility.

A transfer away from prescribing lithium poses the chance of many sufferers lacking out on its potential advantages.
Assertion of pursuits
No conflicts of curiosity to declare.
I’m at present in receipt of PhD fellowship funding via a Wellcome Belief-funded examine in bipolar dysfunction, sleep and circadian rhythm (www.ambientbd.com).
Hyperlinks
Main paper
Ermis, C., Taipale, H., Tanskanen, A., Vieta, E., Correll, C. U., Mittendorfer-Rutz, E., & Tiihonen, J. (2025). Actual-world effectiveness of pharmacological upkeep remedy of bipolar melancholy: a within-subject evaluation in a Swedish nationwide cohort. The Lancet Psychiatry.
Different references
Alsaif, M. (2017). Antidepressants for bipolar melancholy. Nationwide Elf Service. https://www.nationalelfservice.internet/mental-health/bipolar-disorder/antidepressants-for-bipolar-depression/
Baldessarini, R. J., Vázquez, G. H., & Tondo, L. (2020). Bipolar melancholy: a significant unsolved problem. Worldwide journal of bipolar problems, 8(1), 1. https://doi.org/10.1186/s40345-019-0160-1
Edward, D., & Ahmed, S. (2019, 14 June 2019). Prescribing lithium for bipolar dysfunction: are we too scared? The Psychological Elf. https://www.nationalelfservice.internet/mental-health/bipolar-disorder/prescribing-lithium-bipolar-disorder/
Forte, A., Baldessarini, R. J., Tondo, L., Vázquez, G. H., Pompili, M., & Girardi, P. (2015). Lengthy-term morbidity in bipolar-I, bipolar-II, and unipolar main depressive problems. J Have an effect on Disord, 178, 71-78. https://doi.org/10.1016/j.jad.2015.02.011
Kalfas, M. & Leeks, P. (2024). Jury stays out on antidepressant-induced mania. Nationwide Elf Service. https://www.nationalelfservice.internet/mental-health/bipolar-disorder/antidepressant-induced-mania/
Lyall, L. M., Penades, N., & Smith, D. J. (2019). Modifications in prescribing for bipolar dysfunction between 2009 and 2016: national-level knowledge linkage examine in Scotland. The British Journal of Psychiatry, 215(1), 415-421. https://doi.org/10.1192/bjp.2019.16
McIntyre, R. S., Berk, M., Brietzke, E., Goldstein, B. I., López-Jaramillo, C., Kessing, L. V., Malhi, G. S., Nierenberg, A. A., Rosenblat, J. D., & Majeed, A. (2020). Bipolar problems. The Lancet, 396(10265), 1841-1856. https://doi.org/10.1016/S0140-6736(20)31544-0
NICE. (2014). Suggestions | Bipolar dysfunction: Evaluation and Administration | Steerage | NICE. Nationwide Institute for Well being and Care Excellence. https://www.good.org.uk/steering/cg185
Pacchiarotti, I., Bond, D. J., Baldessarini, R. J., Nolen, W. A., Grunze, H., Licht, R. W., Publish, R. M., Berk, M., Goodwin, G. M., & Sachs, G. S. (2013). The Worldwide Society for Bipolar Issues (ISBD) process pressure report on antidepressant use in bipolar problems. American Journal of Psychiatry, 170(11), 1249-1262. https://doi.org/10.1176/appi.ajp.2013.13020185
Pell, C. (2013). Summing up suicide knowledge in bipolar dysfunction. The Psychological Elf. https://www.nationalelfservice.internet/mental-health/bipolar-disorder/summing-up-suicide-data-in-bipolar-disorder/
WHO. (2019). ICD-10 Model:2019. World Well being Organisation. https://icd.who.int/browse10/2019/en








Discussion about this post